
By Chris Bowling
I hate the coronavirus.
Truer words could not define the country and world’s feelings at this moment; however, they rarely appear so succinct and blunt. But that’s exactly what Bonnie Sarton Mierau hears during weekly counseling sessions with kids at the Attachment and Trauma Center of Nebraska in West Omaha.
They say it. Cry it. Whine it.
“I hate the coronavirus.”
“Summer is going to suck.”
“I miss my friends.”
As the country grapples with economic implosion and halted social activity, calls to national services such as the helpline for the Substance Abuse and Mental Health Services Administration have increased fivefold, according to a report by NPR, causing officials to worry how an already-lacking mental health care system will address pandemic-spurred needs, the severity of which they can’t yet predict.
And while everyone’s feeling added pressure from the coronavirus, mental health officials say children, especially those in unstable homes or with existing mental health issues, might be most at risk.
“I think we’re all unsure of what’s going to happen next,” Sarton Mierau said. “I’m concerned there’s going to be a greater need than can be met, which is why we need to figure out other ways to help each other.”
Unable to see their friends, go to school or participate in normal summer activities, safety nets, routines and expectations for many children were swiftly uprooted, isolating kids at home where mental health crises can more easily go unseen. Nationally, minors made up more than half of calls to a national sexual assault hotline for the first time ever in April, according to the Rape, Abuse & Incest National Network (RAINN). NBC News reported instances of flagged child pornography online more than doubled in March compared to the same time last year.
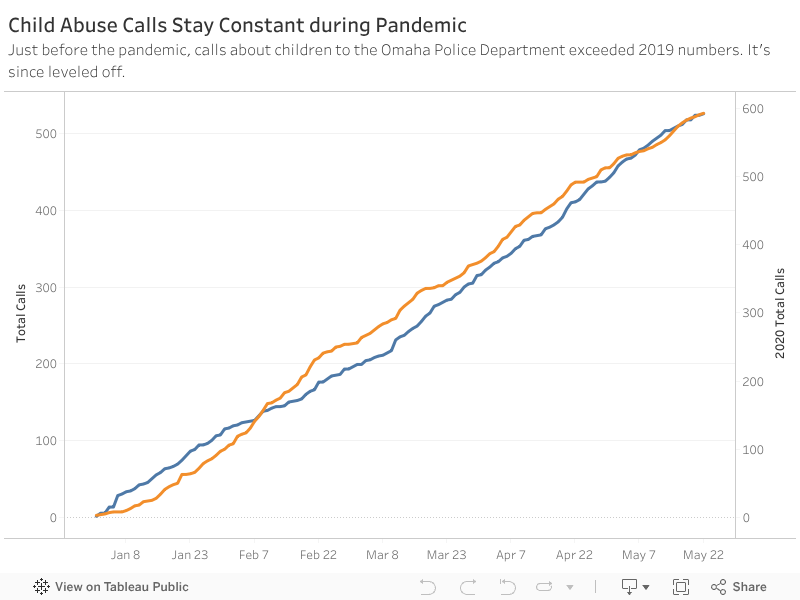
Locally, the Omaha Police Department responded to 18% percent fewer child abuse and neglect reports in March after directed health measures were instituted compared to the same period in 2019, according to the department’s crime data.
That gap has since closed to just 5%, but officials say they believe there’s more out there as families face increased stress. Mental health professionals are also missing out on referrals that would typically come from schools.
“If things don’t change and we stay in this high level of social distancing, my belief is that there will be more abuse and neglect,” said Gene Klein, executive director of Project Harmony, which serves abused and neglected kids in the metro area. “Kids won’t get what they need if family stress continues to be high. We will see more injuries and cases like this.”
Some organizations, such as the Charles Drew Health Center in North Omaha, say they are advertising more, while representatives from Boys Town’s office in South Omaha say they have gone to food banks to hand deliver their information to families in need. But there’s still only so much they can do.
“It is a scary situation, because you want to make sure all kids are safe and that they’re able to go to day care or school or the YMCA if they don’t have an adult keeping an eye on them,” said Regina Costello, director of community support services at Boys Town and the head of its South Omaha office. “The best we can do is keep an eye on the kids we’re working with. It’s really a hard situation.”
The fears of what this might lead to — decreased performance in school and more behavioral health issues — apply doubly to areas where resources were already scarce and more families struggle with poverty. They’re the same areas where minorities are catching the virus at disproportionate rates, in some cases multitudes higher than their share of the population.
But Larry Duncan, senior director of behavioral health services at Charles Drew, doesn’t see the pandemic changing his approach. Trauma from poverty and historic discrimination have plagued North Omaha for decades. A pandemic is just another layer, he said.
The tools he will employ are simple and time-tested: Most importantly, show interest in the life of a child close to you and keep them connected to their community.
“Our focus from the mental health field is to identify what those resiliency factors are and promote that consistently,” Duncan said. “Because that’s not going to change based on the current situation. A problem is a problem no matter what it is.”
What we don’t see
Without kids in schools, day cares, youth groups or any other community hubs, it’s hard to see the effects of the pandemic on kids. Organizations such as Project Harmony, which works with law enforcement to respond to some of the most desperate cases, hope summer months and reopenings will start to reveal what’s been going on behind closed doors, but up until now staff members have felt mostly in the dark.
“Everything has been on pause for many of us,” Klein said. “And we are worried about any slippage that we’ve had in the fight against neglect and getting kids access to mental health care.”
It’s a reality, heightened by the fact Nebraskans of all ages have long struggled to access mental health care in the state. In 2016, per capita rates of psychiatrists in Nebraska were about nine per 100,000 people compared to about 15 for the same population nationally. By 2030, the U.S. Department of Health and Human Services estimates demand for services will overwhelm the supply of most providers.
The strain is felt most acutely in rural Nebraska where rates of psychiatrists were less than a fifth the national average in 2016 and where many counties had no providers at all. Rates are still below average in cities like Omaha and Lincoln, and additional problems include diverse representation.
“Everything has been on pause for many of us. And we are worried about any slippage that we’ve had in the fight against neglect and getting kids access to mental health care.”
– Gene Klein, executive director, Project Harmony
Coupled with a rise in anxiety disorders and depression in kids in recent years, the issues stemming from this pandemic will probably strain an already-lacking mental health care system, said Howard Liu, chair of psychiatry at the University of Nebraska Medical Center.
“It wasn’t enough before, and I don’t think it’ll be enough after,” he said.
Over the past decade, the solution to these issues has been collaboration between mental health organizations, schools, local government and a swath of other partners. Those efforts were led in large part by the Behavioral Health Education Center of Nebraska (BHECN) founded in 2009. From 2010 to 2018, the state added more than 300 people to its mental health workforce. There’s also been an increase of mental health staff in schools as well as deeper training for teachers and community members on how to identify and respond to a child who’s experiencing mental health issues.
The greatest challenge lately has been understanding how the pandemic is affecting kids. From what he’s seen and heard, Liu said he can break it down into three categories.
The kids who were already in crisis or facing poverty, poor relationships with their parents or other issues may be sliding deeper into crisis. The kids who have stable home lives and involved parents are probably doing OK. Then there’s the kids who vary day by day, where sometimes the little things — not seeing their friends, not knowing whether they can attend college in the fall — seem trivial and other days seem catastrophic.
Predicting how that will progress into the future is largely dependent on whether normal routines return, most notably school.
Many districts may be able to reopen on their scheduled calendar days, said Nebraska Education Commissioner Matt Blomstedt earlier this month. But others, such as Omaha Public Schools, have hinted at virtual learning plans this fall, buying more laptops and tablets for kids to use at home. The state also released Launch Nebraska, an online resource to assist at-home learning and provide schools with procedures and guidelines for reopening.
“It is a scary situation, because you want to make sure all kids are safe and that they’re able to go to day care or school or the YMCA if they don’t have an adult keeping an eye on them. The best we can do is keep an eye on the kids we’re working with. It’s really a hard situation.”
The longer kids are away from school and normal routines, the more some worry about the effects of sustained stress and anxiety. After natural disasters, terrorist attacks and other traumatizing events, professionals deploy to help the community cope before the emotions fester into traumatic memories.
The difference with the pandemic is that it’s everywhere, and it’s been happening for months. That troubles Sarton Mierau, because it may be too late for many to get in front of what could be traumatic effects.
“I don’t know how to implement that in this situation, because it’s not over,” she said. “9/11, after a couple weeks, we knew it was over. This is different, it’s ongoing, but there has to be a way that it’s similar.”
Amy Mart, director of professional learning at the Buffett Early Childhood Institute, sees the pandemic differently. It’s affecting adults and kids in less severe ways than other traumatic events, such as chronic violence or natural disasters, she said. But its effects will be prolonged and require officials to approach mental health in a more nuanced and patient way.
“This is a marathon, not a sprint,” Mart said.
There may even be some positive effects. Though they’re juggling more responsibilities, some family relationships might be strengthening with more time inside. Sarton Mierau said many of her younger clients are actually improving with the increased attention they’re receiving now.
The switch to telehealth has also been more seamless than expected for many providers. At Charles Drew, Duncan’s staff saw a slight dip as they transitioned to doing more telehealth. He said they went from about 950 visits in February to 650 in March. However, that increased to around 800 in April, and he expects it to continue to rise as people return for help or new calls come in to set up services.
For Duncan, the challenges brought on by the pandemic are marginal in comparison to the overarching needs of North Omaha.
The federally qualified health center, one of two in Omaha, along with OneWorld in South Omaha, that receive government funding to provide care to underserved communities, has a patient base of which nearly 77% were in poverty and more than half were uninsured in 2018.
Food insecurity and bleak unemployment might be making headlines now, but they’ve been typical for decades here. They’re reinforced by historic trauma, Duncan said, hopelessness backed by years of racism, redlining and violence that sequestered many African Americans to North Omaha without viable options to seek gainful employment, upward mobility or civic representation.
In short, this community has always been on the ropes. There’s no reason to start changing tactics now.
“We don’t need a pandemic to move into gear and now start doing things,” Duncan said. “That’s a different population. That’s not this population. This population already has significant needs.”
The Road Ahead
In the last decade, mental health in Nebraska has seen big improvements, increasing awareness and, in some cases, availability of mental health services as well as connectivity between providers and community gathering places, such as schools.
But there’s still an uphill battle to fight.
“I don’t think anyone believes all the demand is being met,” Mart said. “I think, especially in this current context, that there’s certainly more need than there is ability to serve.”
Charles Drew has set up clinics inside four schools where any student or their siblings can get treated for everything from a sore throat to mental health crisis. In November, the facility also inked a contract to continue providing mental health treatment to detained kids at the Douglas County Youth Center after a pilot program that was a partnership between Charles Drew, Creighton University, CHI Health and UNMC.
“As much as they’ll have us, our goal is already to be available and provide service,” Duncan said.
At Project Harmony, their Connections program has 80 partnerships across the community through schools and medical workers that sync kids with needed mental health care.
Training’s also an important factor in preparing for what may come post-pandemic. Each year, Project Harmony does about 400 training workshops and seminars to help educators and community members spot child abuse, and these have now been moved online. Klein wasn’t sure how receptive people would be to taking the online courses, but so far numbers have been fairly consistent with 700 people utilizing the training in April.

At the Buffett Childhood Institute, Mart said training they’re working on for teachers will have increased focuses on mental health and educating kids dealing with poverty.
“Like we’re seeing with the rise in unemployment,” Mart said, “We’re going to see more economic challenges. There are going to be schools that are going to have to get more serious about [poverty] than they have been in the past.”
In addition to reaching teachers, these types of training seminars reach community partners such as Costello and her staff at Boys Town’s South Omaha office. Costello said they’re making even more use of those learning opportunities now that their caseloads have lessened slightly to prepare for what might come in the next few months.
That willingness to get ahead of the issue was voiced overwhelmingly by those who planned to attend the annual School Mental Health Summit, said Dan Schnoes, chief executive officer at the Educational Service Unit #3, one of many state agencies that oversee and support the long-term goals of several school districts in a particular region.
“Like we’re seeing with the rise in unemployment. We’re going to see more economic challenges. There are going to be schools that are going to have to get more serious about [poverty] than they have been in the past.”
The conference, started by BHECN in 2017, connects mental health professionals, educators and others from across the state to network and share ideas.
Schnoes, who’s co-hosting the conference this year with the Kim Foundation, said organizers considered cancelling the event. But those who signed up said they needed this now more than ever.
“We heard a resounding yes,” he said, “you really need to keep it.”
So far, about 400 people have signed up for the virtual event, which will feature three keynote speakers and 35 breakout panels. That’s lower than what he expected before the pandemic, but all things considered it’s a good sign.
But despite all the training and networking they can do, officials say the best way to curb mental health issues still lies with the adults around the people impacted.
Sarton Mierau said the most important thing a parent can do is to take care of their own mental health so they don’t pass stress on to their child or risk creating an unhealthy living environment. That means reaching out when you need help, taking time to stop reading the news, breathing deeper, going outside and focusing on what you can control right now.
“What kids need to be OK is to see that their attachment figures, their parents, their caregivers, are OK,” she said. “And when they’re OK, [kids] can deal with it.”
If you’re an adult, maybe a neighbor, family member, coach or teacher, who’s forged a relationship with a kid you’re worried about, check in on them.
“That’s all it really takes,” Klein said, “to have one trusted adult they can count on, and their resiliency around a traumatic event like this is pretty powerful.”
And whether you’re a parent or role model, it’s important to know how to talk about the pandemic. Sarton Mierau tells her clients to be honest, but focus on what you know and limit how much information you give them. Younger kids especially are at a stage in brain development where it’s harder to compartmentalize information and discern fact from opinion or immediate dangers from hypothetical ones, she said.
Most important is to know help is available for anyone who needs it. Many insurance providers have waived fees for telehealth services through the pandemic, and even those who aren’t insured can work with facilities such as Charles Drew or OneWorld, which offer sliding-scale payment options that round off costs to meet your income level.
For those who need immediate help, there are national, state and local hotlines where you can talk through what’s going on and be connected with resources.
Nebraska Child Abuse/Neglect Hotline – (800) 652-1999
National Suicide Prevention Hotline – (800) 273-TALK / (800) 273-8255
Nebraska Family Helpline – (888) 866-8660
National Sexual Assault Hotline – 800-656-4673
Hope and Resiliency
The long-term effects of this pandemic on children and their futures are unpredictable.
But the experts we talked to hope this crisis casts a stark spotlight on the importance of investing attention and dollars to treating mental health. They also hope some sense of routine and normalcy returns to kids’ lives this summer and fall.
But getting there will take individual actions.
Taking precautions by wearing a face mask, washing your hands and avoiding large crowds will be vital as the weather warms up and the state reopens many facets of public life. But taking care of our mental health should be just as critical.
Reaching out to someone and asking, “How are you really doing?” Taking care of yourself. Watching out for the people, especially children, who might be struggling. Sarton Mierau hopes that can happen, but wonders how well we can build bridges when even the pandemic has been politicized.
“This really is about focusing more on: How can we help each other learn how to take care of ourselves?” she said. “And I don’t know if that’s a possibility right now.”

Others are optimistic this shared experience will help bring us together.
Klein said it’s uplifting to see mental health professionals rally together. They’re taking training workshops, attending conferences, asking questions and getting involved. In some ways, it’s predictable of an industry that’s always relied on tenacity and resourcefulness to chip away at a problem they’ve never had enough people to solve.
“We remain hopeful we’re going to make it through this,” Klein said, “and that our community is going to be resilient and that we’re going to look back on this period and never forget probably, but it’s not going to define us in any way.”
