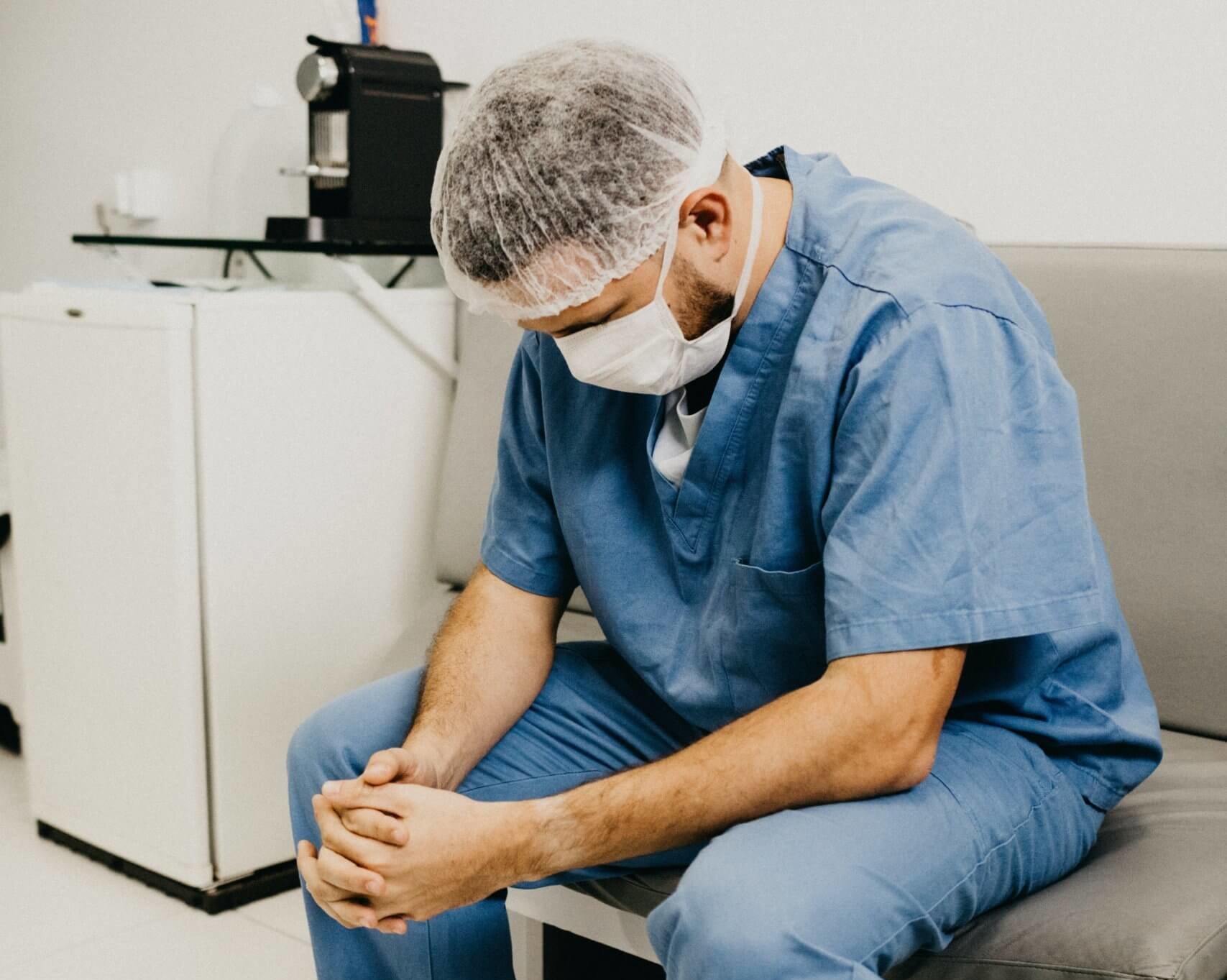
This is the first in a three-part series about the rise of COVID-19 in Nebraska. Check back Friday for the next installment.
By Chris Bowling
If the patient’s lucky, they’ll have a window in their hospital room. Maybe it will be open so they can feel the chill of fall in Omaha, see the falling leaves blow toward Leavenworth Street.
If they’re not lucky, fluorescent lights will beam down as an ICU nurse at Nebraska Medicine slides a tube from their throat, the sound of spit sucked through plastic filling the room.
But chances are they don’t notice much as they’re dying of COVID-19.
They’re given painkillers and anti-anxiety medication as hospital staff turn off the ventilator and the IV. Many have been medically paralyzed for a while, a rarity before COVID-19.
A family member comes in to witness their loved one’s final moments. It could take 30 seconds, 30 minutes or multiple hours. As they wait, there’s a shallow rattle as the person struggles through their final breaths. The sound mixes with shouting and beeping from beyond the glass door as staff try, often unsuccessfully, to save the next person.
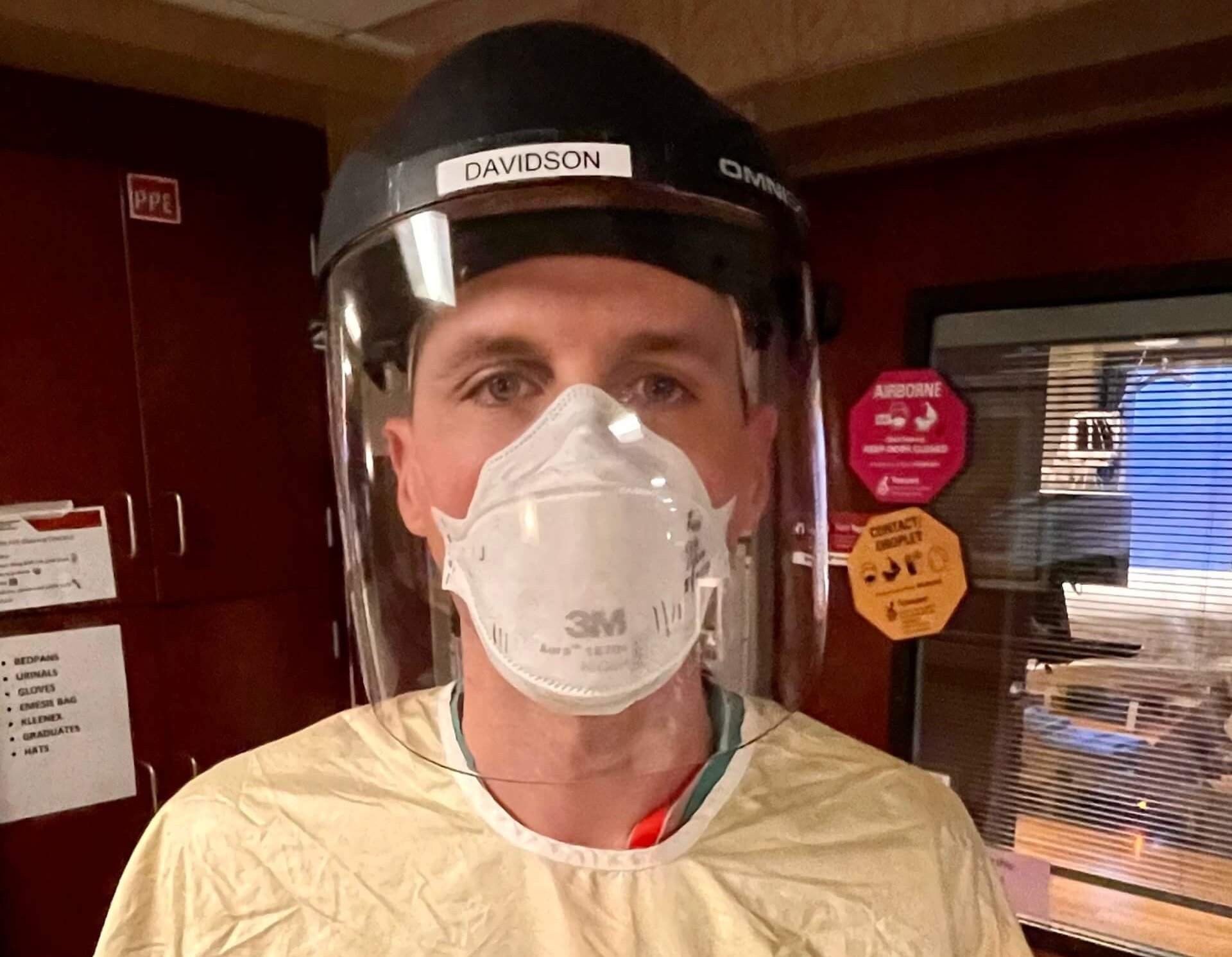
“Those [moments] happen all the time,” said Dr. Ross Davidson, a chief pulmonary and critical care fellow who works in Nebraska Medicine’s COVID ICUs. “They happen every single day.”
Time is something people don’t understand about COVID-19.
While Nebraska reaches 950 deaths from the disease, these are not singular moments. They are weeks watching terrifying infection rates climb higher and higher, days watching a person require more machines to stay alive, hours spent telling family members that their husband, wife, mother or grandfather is going to die. Doctors and nurses work longer and more often just to feel themselves lose control after months fighting this virus every day.
Now hospital staff are begging people to listen: Nebraska is out of time.
“This is real,” said Dr. Kelly Cawcutt, associate medical director of infection control and epidemiology at Nebraska Medicine. “This is absolutely happening in our hospitals. We’re not crying wolf. The wolf is in the house.”
Shadowboxing the Virus
If Nebraska were its own country it’d have one of the highest rates of infection in the world. The state has nearly four times the number of new daily infections it had two months ago. The number of people in the hospital is more than double what it was a month ago and the frequency of deaths has only increased.
If you lined up everyone who’s had COVID-19 since March, they would stretch all the way from Omaha to Grand Island, allowing for six feet of social distancing between people, of course.
And while many COVID metrics have improved in the last week as cities across the state institute their own mask mandates, the rate of infection is still overwhelming hospitals.
While state data shows about a quarter of Nebraska’s hospital beds are still open with an abundance of ventilators, health care workers who spoke to The Reader said an already strained health care system is being pushed to the edge. Not every bed can hold a person with COVID-19, and even as health care workers take on more patients per shift, Cawcutt said they could reach their limits by mid-December if things don’t slow.
“The question is, as we add more COVID units and more teams to take care of these patients, will it be enough?” asked Cawcutt. “Is it possible to even be enough?”
The scariest thing is that Nebraska has already decided its future. New hospitalizations lag reported cases, and in two weeks time, Centers for Disease Control projections put the number of new cases at double what they are today, even though cases are currently decreasing.
Fighting the pandemic, in that sense, is shadowboxing, and Nebraska is losing — its tools to contain the virus becoming either useless or underutilized.
The contact tracers can’t keep up, said Chad Wetzel, a senior epidemiologist with the Douglas County Health Department. Thirty people are on the job locally, the same number since the summer, and up to 250 people statewide can be contracted to help. The time it takes to contact people who’ve tested positive has increased, and trying to create a map of where people got the virus is impossible.
“I think that the only way that we’re most likely going to see a decrease in the rate of transmission is if we see stricter directed health measures,” Wetzel said.
Since declaring a state of emergency in March, Gov. Pete Ricketts has had the authority to close businesses, issue mask mandates and limit public gatherings. But since cases have exploded across the state, he’s done little to reinstate directed health measures since easing them this summer.
Ricketts has also repeatedly opposed a statewide mask mandate. The state’s also threatened legal action against cities or counties who institute their own. Recently, Ricketts announced new directed health measures if COVID-19 patients occupied 25% of the state’s hospital beds. Those would close bars but allow restaurants, churches, salons, gyms and other businesses to continue operating.
And while several cities are starting to declare their own mask mandates, many say the state needs better leadership.
“I would like to give him more credit as an independent thinker and somebody who actually cares about Nebraskans and recognizes that our state can be a leader nationwide and worldwide in finding solutions here,” said state Senator Megan Hunt. “If he would only unmuzzle the public health officials who have the power to give us the guidance.”
Health care workers have started to speak. They’ve started sharing personal stories of fear and exhaustion. They’re tweeting that Gov. Pete Ricketts needs to enact a mask mandate and limit public activity.
And it hasn’t gone unnoticed as national media have written and broadcast their stories. The tweets have been seen across the nation.
But there’s still skepticism. Not only could this amount of spread in Nebraska have been prevented; this is the one place it shouldn’t have happened.
Two years ago, when The Atlantic sought out doctors for a story called “The Next Plague Is Coming. Is America Ready?” it came to the University of Nebraska Medical Center. For years UNMC doctors have been praised as the nation’s leaders in containing new infectious diseases. This is where SARS and Ebola patients were sent.
But that expertise wasn’t enough to guide the pandemic away from the state. And now doctors don’t know if it’ll be enough to stop it.
“I just am dreading the next [few months],” said Dr. Jordan Warchol, the staff physician in Nebraska Medicine’s emergency room. “From now until mid-January, I don’t think anything’s going to get better.”
Check back Friday Nov. 27 for the next installment in this three-part series
