This article was originally published as a three-part series. Read the first in the series here.
By Chris Bowling
If the patient’s lucky, they’ll have a window in their hospital room. Maybe it will be open so they can feel the chill of fall in Omaha, see the falling leaves blow toward Leavenworth Street.
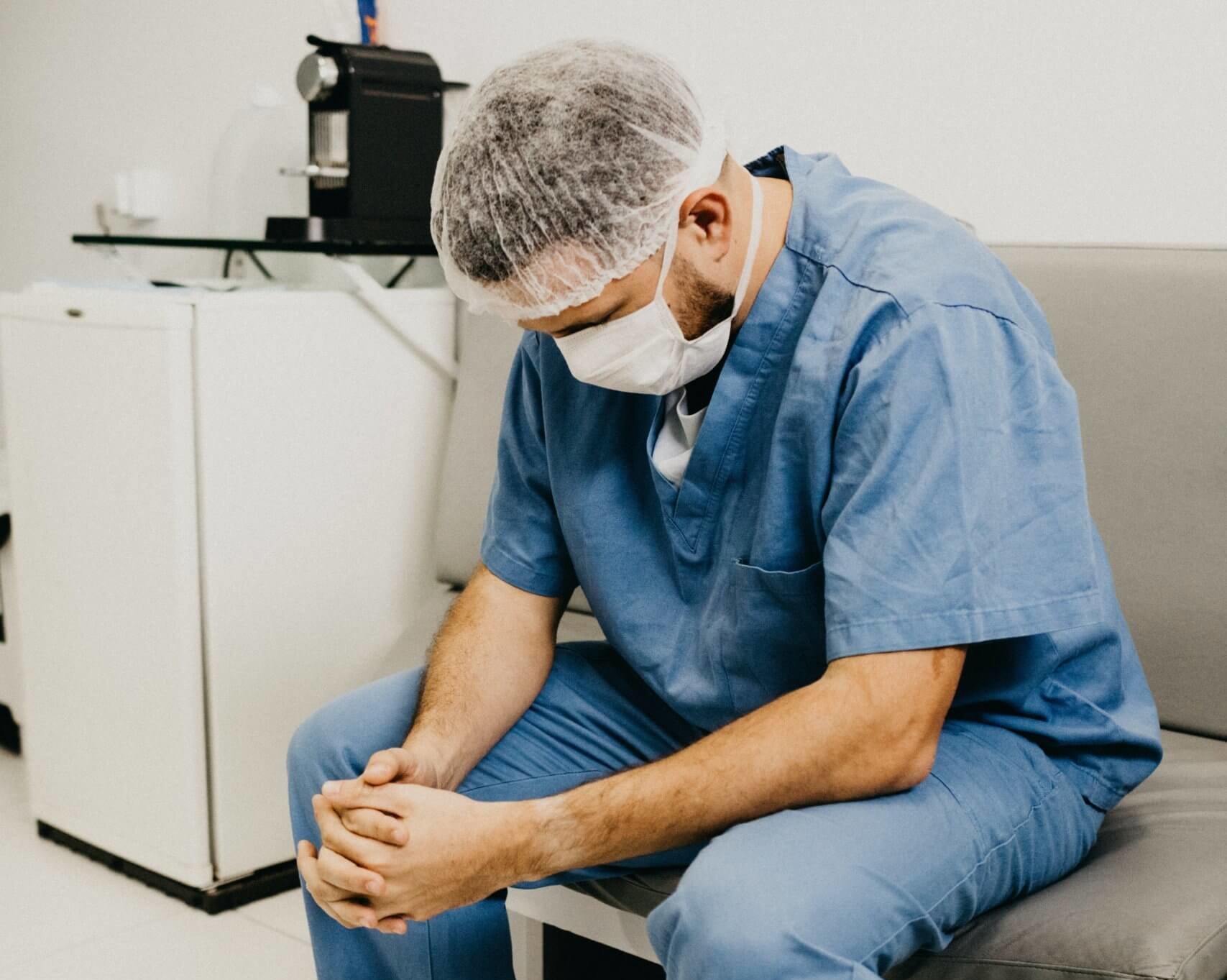
If they’re not lucky, fluorescent lights will beam down as an ICU nurse at Nebraska Medicine slides a tube from their throat, the sound of spit sucked through plastic filling the room.
But chances are they don’t notice much as they’re dying of COVID-19.
They’re given painkillers and anti-anxiety medication as hospital staff turn off the ventilator and the IV. Many have been medically paralyzed for a while, a rarity before COVID-19.
A family member comes in to witness their loved one’s final moments. It could take 30 seconds, 30 minutes or multiple hours. As they wait, there’s a shallow rattle as the person struggles through their final breaths. The sound mixes with shouting and beeping from beyond the glass door as staff try, often unsuccessfully, to save the next person.
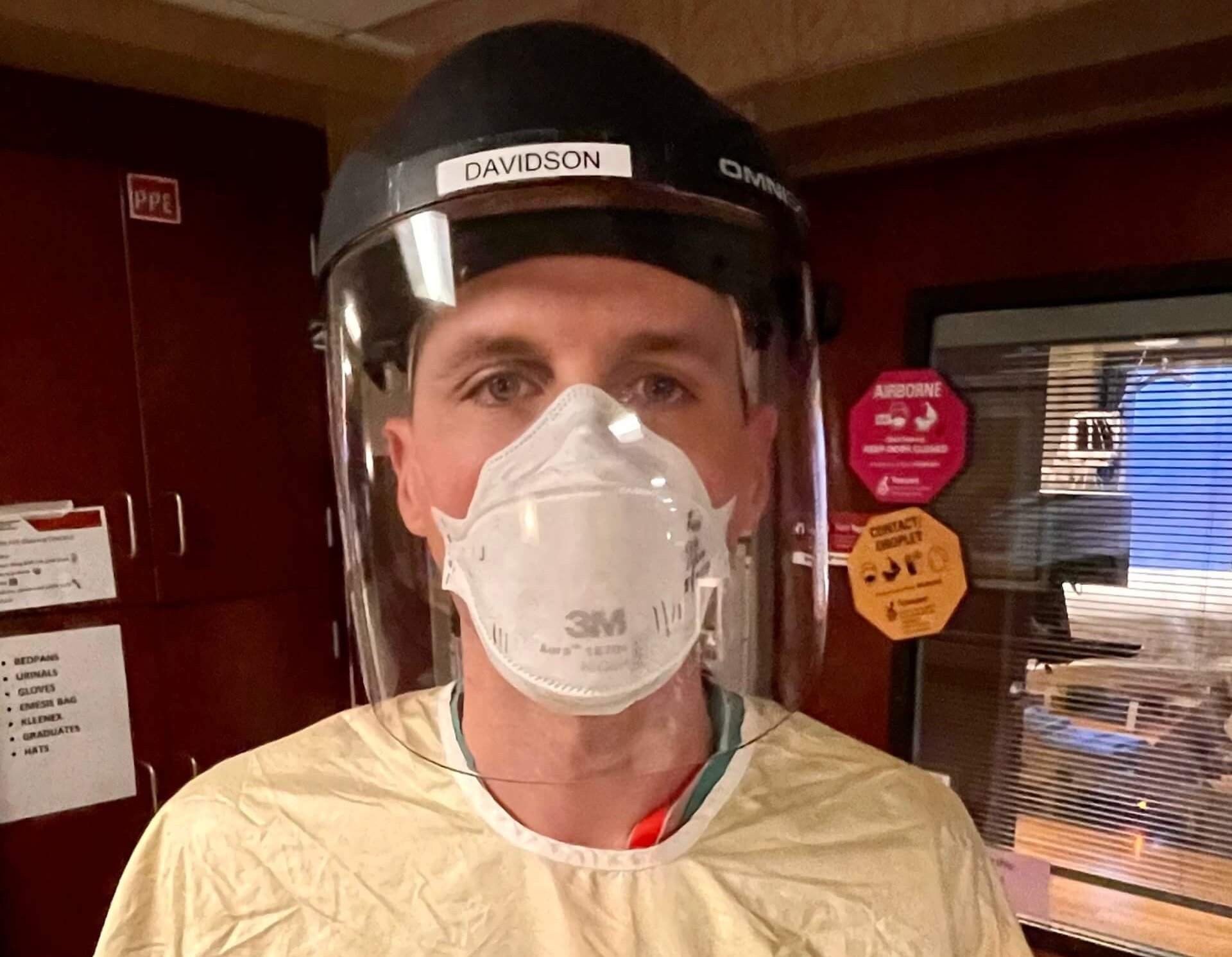
“Those [moments] happen all the time,” said Dr. Ross Davidson, a chief pulmonary and critical care fellow who works in Nebraska Medicine’s COVID ICUs. “They happen every single day.”
Time is something people don’t understand about COVID-19.
While Nebraska reaches 950 deaths from the disease, these are not singular moments. They are weeks watching terrifying infection rates climb higher and higher, days watching a person require more machines to stay alive, hours spent telling family members that their husband, wife, mother or grandfather is going to die. Doctors and nurses work longer and more often just to feel themselves lose control after months fighting this virus every day.
Now hospital staff are begging people to listen: Nebraska is out of time.
“This is real,” said Dr. Kelly Cawcutt, associate medical director of infection control and epidemiology at Nebraska Medicine. “This is absolutely happening in our hospitals. We’re not crying wolf. The wolf is in the house.”
Shadowboxing the Virus
If Nebraska were its own country it’d have one of the highest rates of infection in the world. The state has nearly four times the number of new daily infections it had two months ago. The number of people in the hospital is more than double what it was a month ago and the frequency of deaths has only increased.
If you lined up everyone who’s had COVID-19 since March, they would stretch all the way from Omaha to Grand Island, allowing for six feet of social distancing between people, of course.
And while many COVID metrics have improved in the last week as cities across the state institute their own mask mandates, the rate of infection is still overwhelming hospitals.
While state data shows about a quarter of Nebraska’s hospital beds are still open with an abundance of ventilators, health care workers who spoke to The Reader said an already strained health care system is being pushed to the edge. Not every bed can hold a person with COVID-19, and even as health care workers take on more patients per shift, Cawcutt said they could reach their limits by mid-December if things don’t slow.
“The question is, as we add more COVID units and more teams to take care of these patients, will it be enough?” asked Cawcutt. “Is it possible to even be enough?”
The scariest thing is that Nebraska has already decided its future. New hospitalizations lag reported cases, and in two weeks time, Centers for Disease Control projections put the number of new cases at double what they are today, even though cases are currently decreasing.
Fighting the pandemic, in that sense, is shadowboxing, and Nebraska is losing — its tools to contain the virus becoming either useless or underutilized.
The contact tracers can’t keep up, said Chad Wetzel, a senior epidemiologist with the Douglas County Health Department. Thirty people are on the job locally, the same number since the summer, and up to 250 people statewide can be contracted to help. The time it takes to contact people who’ve tested positive has increased, and trying to create a map of where people got the virus is impossible.
“I think that the only way that we’re most likely going to see a decrease in the rate of transmission is if we see stricter directed health measures,” Wetzel said.
Since declaring a state of emergency in March, Gov. Pete Ricketts has had the authority to close businesses, issue mask mandates and limit public gatherings. But since cases have exploded across the state, he’s done little to reinstate directed health measures since easing them this summer.
Ricketts has also repeatedly opposed a statewide mask mandate. The state’s also threatened legal action against cities or counties who institute their own. Recently, Ricketts announced new directed health measures if COVID-19 patients occupied 25% of the state’s hospital beds. Those would close bars but allow restaurants, churches, salons, gyms and other businesses to continue operating.
And while several cities are starting to declare their own mask mandates, many say the state needs better leadership.
“I would like to give him more credit as an independent thinker and somebody who actually cares about Nebraskans and recognizes that our state can be a leader nationwide and worldwide in finding solutions here,” said state Senator Megan Hunt. “If he would only unmuzzle the public health officials who have the power to give us the guidance.”
Health care workers have started to speak. They’ve started sharing personal stories of fear and exhaustion. They’re tweeting that Gov. Pete Ricketts needs to enact a mask mandate and limit public activity.
And it hasn’t gone unnoticed as national media have written and broadcast their stories. The tweets have been seen across the nation.
But there’s still skepticism. Not only could this amount of spread in Nebraska have been prevented; this is the one place it shouldn’t have happened.
Two years ago, when The Atlantic sought out doctors for a story called “The Next Plague Is Coming. Is America Ready?” it came to the University of Nebraska Medical Center. For years UNMC doctors have been praised as the nation’s leaders in containing new infectious diseases. This is where SARS and Ebola patients were sent.
“UNMC is experiencing what hospitals throughout the Midwest are experiencing—packed facilities, exhausted health-care workers, and grim weeks ahead,” said Ed Yong, a reporter who’s been covering the pandemic in The Atlantic. “But what makes UNMC special is that it, more than any hospital in the country, had specifically prepared to face down a pandemic. The fact that they’re struggling shows that no hospital can prepare for a pandemic that an incompetent president and lax governors allowed to run unchecked.
But that expertise wasn’t enough to guide the pandemic away from the state. And now doctors don’t know if it’ll be enough to stop it.
“I just am dreading the next [few months],” said Dr. Jordan Warchol, the staff physician in Nebraska Medicine’s emergency room. “From now until mid-January, I don’t think anything’s going to get better.”
‘A Slap in The Face’
When Amanda Pappas thinks about how bad the pandemic could get, her thoughts turn to nightmares.
The COVID ICU nurse talked to a doctor recently who wondered whether hospitals would need to commandeer the CHI Center in downtown Omaha. These days it’s common to see people waiting for a bed in the emergency room.
Pappas wonders will they need refrigerated trucks to hold all the dead bodies? Will she ever have to help move someone out of the hospital because their life is less worth saving than someone else’s?
Meanwhile, she sees the pictures of people in packed bars, dining without masks or walking around grocery stores with their noses exposed.
“It just feels like a slap in the face to all of us that are overworked and tired,” Pappas said, who transferred to the COVID ICU in August, “just taking care of these patients all the time for them to act like it’s not that big of a deal or some people are still claiming that it’s fake.”

Mindy, a COVID ICU nurse in Council Bluffs who asked her last name not be included, tested positive for COVID-19 on Nov. 14. She’s worked to exhaustion and broke down crying while praying with patients who are dying alone. She feels like they’re not getting the help they need from the public, the government or even her own hospital.
“I feel like we’ve been — sorry — we’ve been shit on,” she said.
Lisa Ulrich Walters, president of the Nebraska Center for Nursing, said the pandemic is having a huge impact on an already-stretched-thin nursing population. The organization, established in 2000 to address the state’s nursing shortage, projects that the state has about 4,192 fewer nurses than it needs — that number is probably higher because many nurses work less than full time.
Walters said they don’t keep track of how many nurses have left the field in recent months, but she and others interviewed for this story said hospital units have felt the impact of nurses quitting or transferring.
And while Ricketts has reiterated his support to frontline health care workers and added funds to help bolster infrastructure and hire more traveling nurses, the emotional effects can not be easily remedied.
“They’re just doing what has to be done in the time of an emergency,” Walters said. “But at some point in an emergency with that high adrenaline, usually it’s short-lived, you have to stop to process it, deal with that situation, and this isn’t OK. And so the risk is that people end up with post-traumatic stress disorder.”
The emotional toll health care workers have taken over the past nine months sting even more because of the efforts taken to make sure something like this wouldn’t happen.
Cawcutt said planning for the pandemic began in January. At that time, officials at UNMC and Nebraska Medicine knew they’d probably need more beds than the 10 in the hospital’s biocontainment unit.
They didn’t imagine having 10 COVID units across the medical school’s campus. That includes an entire tower dedicated to COVID, three separate COVID ICUs and one unit for people to die in peace. But staff has managed to adjust, bringing in beds, adding additional teams to handle the patients.
Doctors like Davidson have also become more adept at treating the illness. Drugs are more available. Steroids give people’s bodies a better chance at fighting the complications of COVID-19. But maybe the most telling experience health care workers have picked up is being able to tell when someone cannot be saved.
“You get them and they’re on a ton of oxygen, but they’re able to speak with you,” Davidson said. “You see them every day. You watch their oxygen levels progress, and you see, and they know … They know that they’re at risk to die, and they’re scared to death. You’re scared with them.”
In Nebraska, deaths are about a fourth of hospitalizations. Some are discharged from the hospital without ever needing a ventilator. Some leave with holes in their throats where a tracheostomy tube allows them to breathe. Some tell doctors not to resuscitate them if they go into cardiac arrest.
Others don’t understand what doctors are trying to tell them. Davidson has spent hours shouting through a face mask and face shield, over the whine of machines, to patients, trying to explain that a person will die if they don’t let the hospital push a tube down their throat.
Sometimes these conversations take place through a translator. The patient looks at him, speaking a language they don’t understand, dressed like a visitor to an alien world, telling them they will die. They don’t believe him. And then, many of them die.
“If you see one of our COVID patients suffer and pass away,” Davidson, “I just have to believe that you would not be a person, politician or whoever that would continue to believe that general public health, COVID mitigation efforts are wrong.”
Some wonder if it’s possible for the message to ever get across. For months the language has stayed the same — wear a mask, wash your hands, socially distance, stay home if you can — and still people fight it. Some don’t even accept the science after it’s too late.
When a friend of Warchol’s had to tell the family of one man that he had died of COVID-19, they responded:
“There’s no way he could’ve died from COVID, because COVID isn’t real.”
‘Our Hands Are Tied’
Tony Vargas doesn’t do well feeling defeated. The state senator representing District 1 in South Omaha can deftly flip any situation on its head to see opportunity and solutions.
But if anything could challenge that optimism, it’s COVID-19.
In April, he was in New York City, watching his father, Antonio Vargas, die after catching the virus. Weeks later Vargas was back in Nebraska watching his bill to protect meatpacking workers, hard-hit by the virus, flounder. Senators refused to wear masks, and recently Sen. Mike Groene of North Platte announced he “got his wish” by catching the virus, a step toward herd immunity.
A video was shared online showing Ricketts, who’s talked up masks in press conferences, not wearing a mask in a crowded Omaha bar. The server who shot the video was fired. On Twitter, Taylor Gage, the governor’s spokesman, insinuated doctors calling for stronger health health measures did so because of their political views.
Just like most places in America, COVID-19 has become a political issue that Vargas, and many other politicians, can do little about.
“It frustrates me that our hands are tied to do that,” he said. “But I also recognize that the governor is able to do something about it, and he’s choosing not to utilize this tool that could potentially save more lives.”

Since Ricketts declared a state of emergency, Vargas said he and other senators have tried to lobby the governor for stronger health measures, but to little effect.
The strategy now is grassroots advocacy: retweeting doctors sharing harrowing stories inside COVID ICUs, trying to build coalitions with business owners and changing public health from the bottom up.
“We’ve seen Iowa move in new ways and that happens because of elected officials or everybody working in concert to say that we need to do more,” he said. “We saw that in North Dakota, we’ve seen that in Utah, and it really gives me hope, it really does.”
And now city’s around the state are chiming in. Norfolk, Gretna and Ralston have all instituted mask mandates while Lancaster County has rolled back on public health measures without the Governor’s permission.
For others like Senator Megan Hunt it’s so little so late. It doesn’t mean they stop trying, but the fact that working class people and the most vulnerable have had to find solutions for these problems is unacceptable.
“[Those in power] know that they can leave the workers and the poor and the vulnerable among themselves to support each other with their little food banks and their clothing drives and their GoFundMe,” she said. “A nation and a state that depends on GoFundMe to keep people housed, to keep people healthy, to keep children fed, is a broken state.”

Hunt wants people to take note of how elections contribute to these situations. Because of the legislature’s political makeup, something she attributes to the $1.8 million Ricketts has personally spent in the state, it’d be impossible to gather the 33 of 49 senators to call a special session to put decision-making tools back in their hands, Hunt said.
Vargas hopes people see that, too, but he also wants them to see mounting public pressure change the governor’s mind. Either way, it’s just not an option to quit, he said, especially when things are so dire.
Vargas thinks back to April. His dad was unconscious for 29 days. He had a collapsed lung and two incisions along his abdomen. He was 100% reliant on a ventilator. His mom, older brother and nephew were bedridden with the illness. And then his dad died. If he shut down then, no one would have blamed him.
But he thought about his parents. They were immigrants to this country who had nothing, didn’t know the language and had no job. They fought against so many odds to make a life for him and his brothers. He owed it to them to keep going.
“I haven’t reached my breaking point yet, and I really hope I don’t,” Vargas said. “But if my parents, my mother, can get through this then I have to do everything I can to maintain a level head and keep fighting. That’s what I signed up for.”
An Uphill Battle Ahead
Time isn’t stopping for COVID-19.
Every day the sun sets and Amanda Pappas gets a skinny vanilla latte from Scooters before her night shift. It’s her one pick-me-up before she goes into the COVID ICU where so many don’t leave.
As the sun rises, Dr. Jordan Warchol walks into an already busy emergency room where people stand waiting for beds.
Days pass and Dr. Kelly Cawcutt watches while no new directed health measures come. As weeks turn to months, Lisa Walters wonders how much more health care workers can take.
Because the worst case scenario keeps getting surpassed and the nightmares seem just around the corner. Still, doctors need to adapt. If there is a breaking point, Dr. Ross Davidson said, he’ll lose something inside of him, but he’d never stop showing up to work.
“I think that we have an uphill battle ahead,” he said. “I think that if we want that uphill battle to be less steep, we’d have to change things now, like literally tomorrow. I don’t think it’s going to happen. So what I’m personally preparing for is a pretty long winter with a lot of work and a lot of seeing a lot of people be very sick and die.”