This story was originally published by Nebraska News Service.
HASTINGS – With two nurses out sick in early December, charge nurse Osa Brooks found herself scrambling to care for 28 patients. With only one floor nurse available, employees from other units were called in to work the floor or give medications.
“It was really scary because I had 10 patients that I was responsible for, and I had another nurse giving medications for me,” Brooks said.
Brooks said the chaos scared her because of the chance that she could have missed something, causing her patients a longer stay at Mary Lanning Memorial hospital or impacting the level of care they received.
According to the Nebraska Department of Labor, as of Dec. 21, 2021, the resident nurse assistant occupation is the most highly advertised position online with 3,068 job openings, followed closely by nursing assistants and licensed practical and vocational nurses.
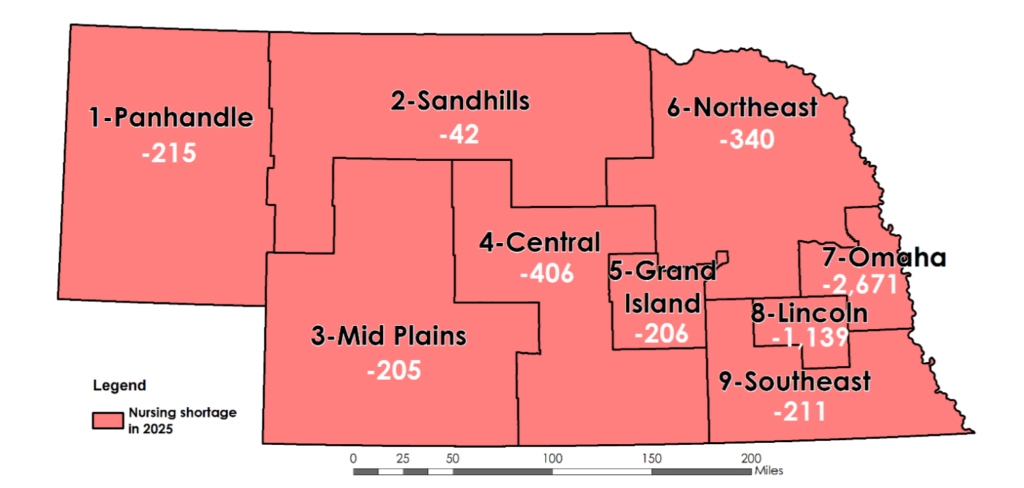
Depicts the projected nursing shortages by region of Nebraska in 2025.
A licensed practical nurse, also known as a licensed vocational nurse, is a healthcare professional that provides basic nursing care.
The difference between an LPN and an RN is the level of education: an LPN attends school for about one year, while an RN receives a two or four-year degree in nursing science.
Ronda Ehly, chief nursing officer and administrator at Mary Lanning Memorial in Hastings and a member of the Center for Nursing Board, said that nursing coverage is sparse across Nebraska. The 533 R.N.s in Adams County, work at critical access hospitals, licensed long-term care facilities, clinics and so forth. Mary Lanning Memorial hospital alone has more than 200 nurses, according to Ehly.
“Buffalo County has 930 R.N.s and Hall has 719,” Ehly said. “When you look at those tri-cities, and there’s five hospitals in those Tri-City areas, it’s kinda insane.”
The Tri-Cities of Nebraska are Grand Island, located in Hall County; Hastings, located in Adams County; and Kearney, located in Buffalo County.
The Nebraska Center for Nursing – a Department of Health and Human Services organization created by the Nebraska Legislature to address the nursing shortage in the state – analyzes workforce data, collaborates with schools and companies to elevate the competency of the current workforce and promotes the nursing profession.
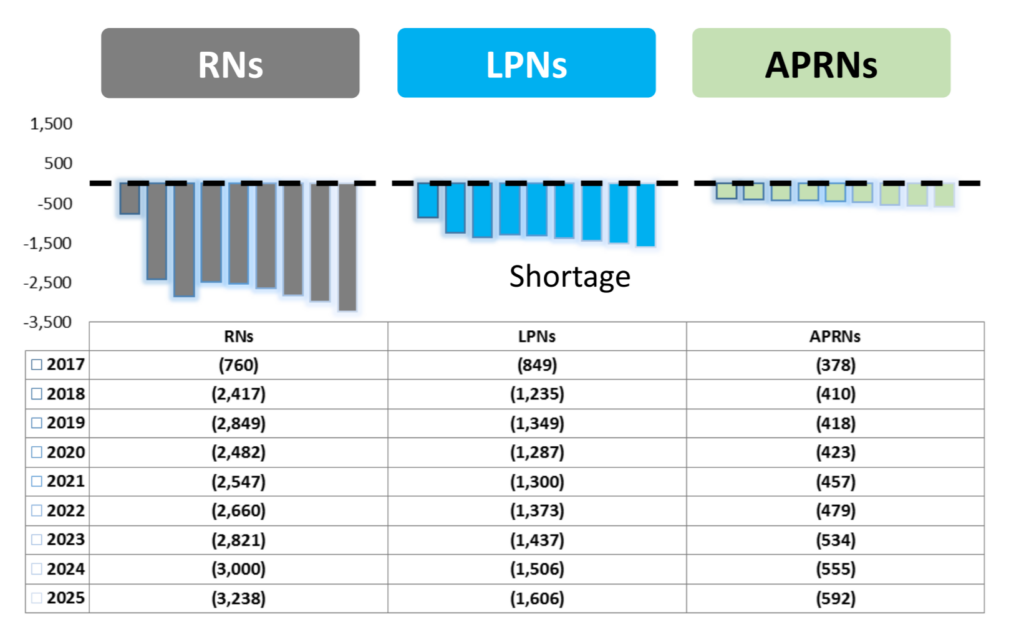
The CFN projects a nursing shortage of 5,345 full-time nurses by 2025, according to its 2017 workforce model. This number combines predicted resident nurse, licensed practical nurse and advanced practice registered nurse gaps.
The need for nurses is so great that hospitals are advertising to nurses who are already employed.
“I’ve gotten advertisements in my email left and right for me to go somewhere else,” Brooks said. “I haven’t even applied anywhere; I’m not looking.”
According to Ehly, Nebraska isn’t producing enough new nurses to offset the number of those retiring. The average age of nurses in Nebraska is 44. At Mary Lanning Memorial specifically, 22% of the workforce is over the age of 60.
Several years ago, Ehly projected 22 retirements over a three-year period, a number that held true.
COVID-19 worsened the already existing staffing challenge.
“Our hospitals here in Nebraska are facing one of the, if not the, most challenging times of the pandemic. COVID-19 positivity rates are racing upward and hospitalization rates are following,” said Jeremy Nordquist, president of the Nebraska Hospital Association, in a Jan. 10 press conference. “We could see a doubling of hospitalizations due to covid in Nebraska over the next two to three weeks. That alone would overwhelm our healthcare system but we’re also facing some of the worst staffing challenges we’ve had during COVID-19.”
Nordquist said that the challenges of hospitalization rates and workforce shortages exist border to border in Nebraska.
“Our supply of healthcare workers and beds is being outstripped by the demand for care and services,” said Todd Consbruck, president and CEO of Avera St. Anthony’s and Avera Creighton hospitals, in a Jan. 10 press conference. “This new variant is happening very quickly and taking our workforce out along with it.”
According to Brooks, Mary Lanning Memorial had a full staff at the beginning of the pandemic. Most patients didn’t come into the hospital unless they absolutely had to and postponed elective surgeries. Now the nurses need to take care of the COVID-19 patients in addition to offering other routine care.
“It seems like there’s a lot more patients who’ve been sick than there was before,” Brooks said. “People were holding off to see if everything would get good and some of them waited too long.”
According to Brooks, nurses close to retirement decided to leave earlier than originally planned, not wanting to deal with the extra stress of the current situation. Others transferred to doctors’ offices or traveling nurse agencies. Some left the healthcare profession entirely due to burnout or other reasons, Brooks said.
Caring for COVID-19 patients requires additional time due to sanitation protocols and the need to don personal protective equipment, adding additional strain, Brooks said.
According to Ehly, community-acquired breakouts of COVID-19 have also occurred among the staff, an issue seen in other hospitals as well. Nearly 200 Nebraska Methodist employees are currently out with COVID-19, 50 of which are nurses.
“Our chambers are not airtight against the walls in those rooms [with COVID-19 patients],” said Kerensa Anderson, a registered nurse at Mary Lanning Memorial.
Anderson said that the hospital has relocated recovering COVID-19 patients to other hospital areas outside of the intensive care and progressive care units where they remain in quarantine.
In the past three months, nurses have taken up to six COVID-19 patients per day, in addition to their other patients, Anderson said.
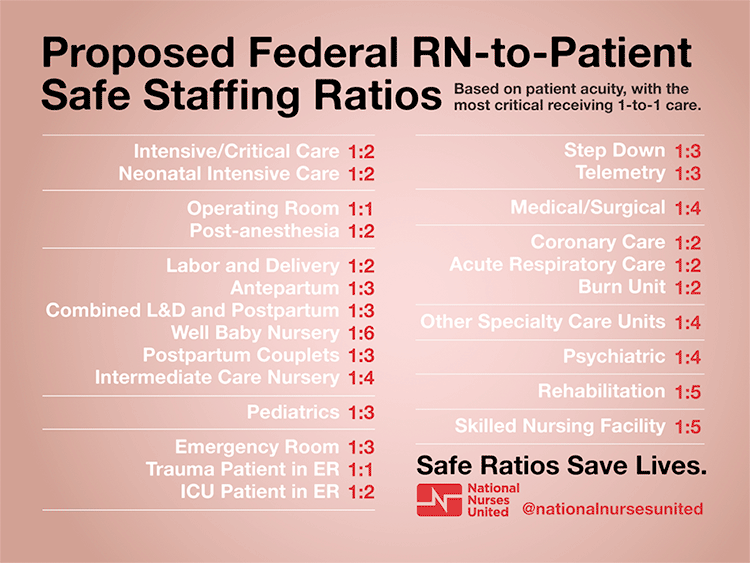
The supply of nurses directly affects the number of patients each is responsible for. Although 49 states have no legal cap on the patient-nurse ratio, National Nurses United advocates for a maximum number of patients per nurse, which varies per department, in order to ensure patient safety and quality care.
For medical/surgical units, NNU’s optimal ratio is four patients per nurse.
“We always were really well known for having great staffing ratios,” said Anderson. “Now there are times when, even on good days, we take eight to 10 patients per nurse. And before we were seeing three to five. It is not adequate, it is dangerous.”
According to Anderson, nurses in Mary Lanning Memorial’s medical/surgical unit are working 13-15 hour shifts and some are working four or five days a week. Typically, nurses work three, 12-hour shifts a week or five, 8-hour shifts.
“Honestly, for as long as I’ve been at Mary Lanning, it’s never ever been just 12 hours. You don’t just get to clock in and clock out when that 12 hours is up,” Anderson said. “They are 13-15 hour days. And you have to turn around and do it again the next day and the next day and the next day on little food, on little sleep.”
Ehly said that Mary Lanning Memorial is requiring staff to pick up extra shifts, but has tried to limit it to one shift every two weeks by enlisting travel nurses and agency staff to support them.
Nurse agencies employ travel nurses in hospitals in need of extra staff. Over 300 agencies exist across the country, with agencies in every state. Agencies find assignments for nurses in the area they are interested in, show the nurses the pay and benefits of different opportunities and, if a nurse decides they are interested, submit an application on the nurse’s behalf.
The hospital follows up with the nurse to set up an interview and create a contract. Most places that employ agency staff offer a 13-week contract that can be extended to a total of one year.
“Even in the worst of times, we’ve had maybe three or four agency staff,” Ehly said. “We’re up to 17, throughout the house.”
According to Ivan Mitchell, CEO of Great Plains Health in North Platte and 2020 Board Chair for NHA, in a Jan. 10 press conference, hospitals previously tried to limit the amount of agency staff due to high costs. At this point, they struggle to even find available agency staff, Mitchell said.
“We are tired, we’re making mistakes, we are getting sick. We don’t have time to eat or use the bathroom or take drinks of water,” Anderson said. “We run all day. Sometimes we don’t get lunches. Sometimes we do maybe get to sit for five to 10 minutes.”
In early December, Mary Lanning Memorial provided a Christmas meal for the staff. The food was brought up to the medical/surgical unit around noon. Brooks wasn’t able to eat until 8:30 p.m. because she wasn’t able to take a break due to the lack of staff.
“Some people just don’t eat at all until they go home,” Brooks said. “We all have more patients than we can handle right now.”
According to Anderson, between giving meds, checking on patients and communicating with doctors and hospitals, the nurses are running constantly. Sometimes there are only three or four nurses on the floor and one or two aides, if any.
Tonya Elley, a travel operating nurse employed by the TotalMed agency, said that this time of year, October through December, has traditionally been the busiest time of year for surgery as people try to get procedures done if their insurance deductibles are met.
“With the busy time of surgery, the floors are also getting those patients,” Elley said.”Then also obviously with the pandemic and the lack of beds, we’ve had to hold patients in the recovery room because there’s no floor beds. Some of it has to do with staffing.”
Administration assigns staff from other areas to assist the medical/surgical unit, but they need time to learn the resources on the floor and how to function in that team setting, Ehly said.
“You just keep going because you don’t have a choice,” Anderson said. “It’s just hard on everybody because of the demands. And we’re doing it with less staff.”
According to Elley, this issue is not isolated to Mary Lanning Memorial. She’s worked as a traveling nurse at three Nebraska locations and one in Iowa over the past two years. Elley is about to start her fourth placement in Nebraska.
Elley said that conditions across the hospitals are similar. The nurses are overworked, and the administrators try to employ travel nurses to ease the burden.
“We still pretty much always get our 30-minute break, but we don’t always get our 15-minute breaks,” Elley said. “Floor nurses are worse off in that area.”
With the hectic pace at the hospital, nurses miss being able to slow down and talk to their patients.
“A lot of us miss the days when we could really interact with our patients and talk and give them uplifting or emotional support, rather than just running in and out of the room,” Anderson said. “That’s the part of nursing we all miss. We’re all hoping that someday things slow down a little bit and we can have a little piece of that back.”
According to Anderson, nursing is more than giving meds and keeping patients alive. It is also about connecting with another human being and giving needed advice.
“We have so many patients; we’re so rushed we’re not able to give that part of ourselves,” Anderson said. “We just feel like robots, dispensing meds and doing everything that we have to do, rather than some of the things that we miss doing.”
Ehly said that the quality of patient care has not declined and that the hospital monitors patient outcomes carefully. However, she said, the nurses feel they are lacking the ability to connect personally with patients.
“They just feel like they’re going from patient to patient, and they’re doing all the things they need to do to keep them safe, that’s their focus,” Ehly said. “But it takes away from some of that time to just sit down and say, ‘So, how are you doing today?’”
Additionally, Ehly said nurses are disheartened by the change in attitude from some patients, especially when working in tough conditions.
“A year ago, or even more than a year ago, nurses and healthcare workers were touted as heroes,” Ehly said. “They were drawing pictures on the sidewalk, sending notes and things. And now, as my boss said in an article in the [Hastings] Tribune, we’ve gone from heroes to zeroes.”
According to Ehly, people are taking their frustrations out on healthcare workers, some of which are related to staffing levels.
“We do not condone disrespectful behavior to our staff,” Ehly said. “I’ve had to go talk to patients or families or give them a call and say ‘Listen, I know you’re stressed, I know you’re scared, but these people are taking care of your loved one and they’re doing a great job. You need to give them the respect they deserve.’”
Other hospitals in Nebraska echoed Ehly’s concerns.
“Nebraska as a whole is a caring and compassionate group, but we are seeing segments of society right now who are not giving healthcare workers the respect and kindness that they deserve,” Consbruck said.
According to Ehly, some nurses have retired early or left healthcare altogether due to the current conditions.
“I love being a nurse,” Brooks said. “That’s what I’ve always wanted to do. And I still love taking care of patients, but there’ll be a point where I can’t do it this way anymore.”

